More than ever, patients are engaged in their medical care, which is encouraging when you consider most medical school mission statements emphasize patient communication and education. It’s also worth noting that research shows providers are able to drive positive patient outcomes using a teach-back method that involves caring and clear language. Yet even well-informed individuals lack some knowledge, such as the distinction between inpatient versus outpatient care.
So what’s the difference, and why does it matter? This overview can help you advance your health literacy.
Inpatient vs. outpatient: Distinguishing the differences in care
What is an inpatient? In the most basic sense, this term refers to someone admitted to the hospital to stay overnight, whether briefly or for an extended period of time. Physicians keep these patients at the hospital to monitor them more closely.
With this in mind, what is outpatient care? Also called ambulatory care, this term defines any service or treatment that doesn’t require hospitalization. An annual exam with your primary care physician is an example of outpatient care, but so are emergent cases where the patient leaves the emergency department the same day they arrive. Any appointment at a clinic or specialty facility outside the hospital is considered outpatient care as well.
While there’s a clear difference between an inpatient and an outpatient, there is a little bit of gray area as well. Occasionally, physicians will assign a patient observation status while they determine whether hospitalization is required. This period typically lasts for no more than 24 hours.
Also note that the location itself doesn’t define whether you’re an inpatient versus outpatient. It’s the duration of stay, not the type of establishment, that determines your status.
Inpatient vs. outpatient: Comparing services
You’re probably starting to get a sense of the varying circumstances that fit under each category. To further recognize the difference between inpatient and outpatient care, review the below treatments and services that are common for these two types of care.
Inpatient care examples
- Complex surgeries, as well as some routine ones
- Serious illnesses or medical issues that require substantial monitoring
- Childbirth, even in cases that don’t require a cesarean section
- Rehabilitation services for psychiatric illnesses, substance misuse, or severe injuries
Outpatient care examples
- X-rays, MRIs, CT scans, and other types of imaging
- Lab tests, such as bloodwork
- Minor surgeries, particularly ones that use less invasive techniques
- Colonoscopies
- Mammograms
- Consultations or follow-ups with a specialist
- Routine physical exams
- Same-day emergent care, often treated at an urgent care facility versus the ER
- Chemotherapy or radiation treatment
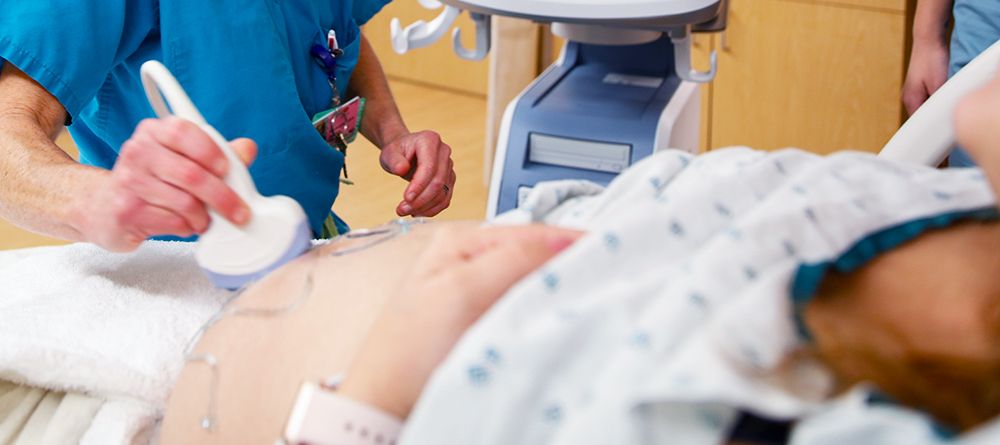
Inpatient vs. outpatient: The providers in each setting
Primary care physicians have traditionally been considered outpatient providers, while specialists are thought of as inpatient physicians. But that’s really an oversimplification, particularly when you consider that hospitalists bridge the gap by providing general medical care to inpatients. Effective care requires that doctors work together and effectively leverage health care technology, regardless of their specialties and settings.
Many physicians also divide their time between inpatient and outpatient services. OB/GYNs, for example, provide inpatient care when delivering babies and outpatient care when consulting with pregnant women during prenatal checkups.
Generally speaking, inpatients have contact with a larger group of providers. During a hospital stay, you could interact with physicians, nurse practitioners, lab technicians, physical therapists, pharmacists, and physician assistants.
Inpatient vs. outpatient: Cost considerations
The difference between inpatient versus outpatient care matters for patients because it will ultimately affect your eventual bill.
Outpatient care involves fees related to the doctor and any tests performed. Inpatient care also includes additional facility-based fees. The most recent cost data included in the Healthcare Cost and Utilization Project from the Agency for Healthcare Research and Quality (AHRQ) shows the average national inpatient charges can vary considerably depending on the length of stay and the treatment involved. The exact amount you pay also hinges on your insurance.
Things get a little more complicated if you have Medicare. Outpatient care and physician-related services for inpatient care are covered by Part B. Hospital services like rooms, meals, and general nursing for inpatients are covered by Part A.
But if you stay overnight in the hospital under observation status, Medicare still considers you an outpatient and will not cover care in a skilled nursing facility. It can certainly be confusing, so don’t be afraid to ask the medical team about your status. They’re used to these types of questions.

Expand your medical knowledge
Hopefully, you now have a little more clarity concerning the definition of inpatient versus outpatient. It can go a long way towards helping you understand what you should expect during and after any sort of medical treatment.
You can further deepen your understanding of the health care world by reading our article “50 Must-Know Medical Terms, Abbreviations, and Acronyms.”
*This article was originally published in June 2019. It has since been updated to reflect information relevant to 2021.


